Source: Science Direct
Abstract
Background
In France, the combination hydroxychloroquine (HCQ) and azithromycin (AZ) is used in the treatment of COVID-19.
Methods
We retrospectively report on 1061 SARS-CoV-2 positive tested patients treated with HCQ (200 mg three times daily for ten days) + AZ (500 mg on day 1 followed by 250 mg daily for the next four days) for at least three days. Outcomes were death, clinical worsening (transfer to ICU, and >10 day hospitalization) and viral shedding persistence (>10 days).
Results
A total of 1061 patients were included in this analysis (46.4% male, mean age 43.6 years – range 14–95 years). Good clinical outcome and virological cure were obtained in 973 patients within 10 days (91.7%). Prolonged viral carriage was observed in 47 patients (4.4%) and was associated to a higher viral load at diagnosis (p < .001) but viral culture was negative at day 10. All but one, were PCR-cleared at day 15. A poor clinical outcome (PClinO) was observed for 46 patients (4.3%) and 8 died (0.75%) (74–95 years old). All deaths resulted from respiratory failure and not from cardiac toxicity. Five patients are still hospitalized (98.7% of patients cured so far). PClinO was associated with older age (OR 1.11), severity at admission (OR 10.05) and low HCQ serum concentration. PClinO was independently associated with the use of selective beta-blocking agents and angiotensin II receptor blockers (p < .05). A total of 2.3% of patients reported mild adverse events (gastrointestinal or skin symptoms, headache, insomnia and transient blurred vision).
Conclusion
Administration of the HCQ+AZ combination before COVID-19 complications occur is safe and associated with very low fatality rate in patients.
Keywords
SARS-CoV-2COVID-19HydroxychloroquineAzithromycin
1. Introduction
COVID-19 is a pandemic, with a rapid global spread of infection since January 2020 [1]. Four studies have demonstrated that hydroxychloroquine sulfate (HCQ) inhibits SARS-CoV-2 in vitro [[2], [3], [4], [5]]. One study has demonstrated that the combination of HCQ and azithromycin (AZ) inhibits SARS-CoV-2 in vitro [6].
Several clinical studies addressing the efficacy of HCQ were conducted in COVID-19 patients leading to contradictory results. Three studies showed a favourable effect [[7], [8], [9]]. A Chinese randomized control trial (RCT) conducted in 62 COVID-19 patients showed a significantly shortened body temperature recovery time, cough remission time and a larger proportion of improved pneumonia as assessed by CT scan in patients treated with 400 mg HCQ per day during five days (N = 31) than in controls (N = 31) [7]. Another Chinese RCT conducted in 150 COVID-19 patients showed significant favourable differences between patients treated with 1200 mg HCQ/day for three days, then 800 mg/day for two to three weeks (N = 75) and controls (N = 75) regarding alleviation of symptoms and decrease of C-reactive protein concentration [8]. An Iranian study conducted in a cohort of 100 COVID-19 patients treated with 200 mg HCQ twice daily (400 mg single dose when combined with administration of lopinavir/ritonavir) concluded that HCQ improved the clinical outcome of the patients [9].
A Chinese RCT conducted in 30 COVID-19 patients showed no significant differences between patients treated with 400 mg HCQ per day during five days (N = 15) and controls (N = 15) regarding pharyngeal carriage of viral RNA at day 7 [10]. A French study conducted in 181 COVID-19 patients with relatively severe illness did not show any difference between 84 patients treated with 600 mg HCQ/day and 97 controls regarding transfer to ICU and death [11]. Finally, a retrospective analysis of data from patients hospitalized with confirmed SARS-CoV-2 infection in all United States Veterans Health Administration medical centers found no evidence that, before ventilation, the use of HCQ either with or without AZ, reduced the need for subsequent mechanical ventilation [12]. None of these studies was perfect. In the Chinese and Iranian studies, patients received multiple additional treatments including antivirals.
A preliminary French non-randomized clinical trial conducted in 36 COVID-19 patients showed a significant reduction in viral nasopharyngeal carriage at day 6 in patients treated with HCQ at 600 mg per day during 10 days (N = 20, 70% testing negative), compared to untreated controls (N = 16, 12.5% testing negative). In addition, of the twenty patients who were treated with HCQ, six received AZ for five days (for the purpose of preventing bacterial super-infection) and all (100%) were virologically cured at day 6, compared to 57.1% of the remaining 14 patients [13]. This synergistic effect is the rationale to use the combination HCQ and AZ.
We recently reported on 80 patients using a combination of 200 mg HCQ three times daily for ten days plus AZ (500 mg on day 1 followed by 250 mg daily for the next four days) with good clinical and virological outcomes [14]. AZ has been shown to be active in vitro against Zika and Ebola viruses [[15], [16], [17]] and more recently against SARS-CoV-2 [5].
In a recent international survey conducted among at least 7500 physicians across 30 countries, most of the questioned physicians considered that HCQ and AZ are the two most effective treatments among available therapies for COVID-19 [18]. Here, we report a retrospective evaluation of 1061 new COVID-19 patients, treated for at least 3 days with HCQ+AZ from the time of diagnosis and a follow up of at least nine days. Outcomes were death, clinical worsening and viral shedding persistence.
2. Materials & methods
2.1. Patients and study design (Fig. 1)
The study was conducted at Assistance Publique-Hôpitaux de Marseille (AP-HM), Southern France in the Institut Hospitalo-Universitaire (IHU) Méditerranée Infection (https://www.mediterranee-infection.com/). We have set up early unrestricted massive PCR screening for patients suspect of COVID-19 and for asymptomatic contacts of confirmed cases. Data was collected on patients included from March 3rd to March 31st. Individuals with PCR-documented SARS-CoV-2 RNA from a nasopharyngeal sample [19], were proposed HCQ+AZ early treatment, as standard care, whether or not they had symptoms, with treatment initiation at our day-care hospital (inpatients) or at our infectious disease units (inpatients) when required. Patients initially treated in the day-care hospital or discharged from conventional hospitalization wards before day 10 were followed in the day-care hospital (ambulatory follow-up as outpatients). Patients were also referred to the IHU from other health care facilities. Patients with at least three days of treatment and nine days of follow-up are described in this analysis. Demographics, chronic conditions and concomitant medications were documented. The patients described in previous studies [13,14] were not included in the present work. On April 18th, a new evaluation of data was done to update fatal cases and case fatality rates.
2.2. Clinical and radiological classification and follow-up
Details are available from our previous studies [13,14]. Briefly, patients were grouped according to clinical presentation at admission (upper respiratory tract infections or lower respiratory tract infections symptoms) and severity was assessed using the national early warning score (NEWS) for COVID-19 patients at admission and during follow-up [20]. We defined three risk categories for clinical deterioration: low score (NEWS 0–4), medium score (NEWS 5–6), and high score (NEWS≥7). The time between the onset of symptoms and treatment was documented. Patients underwent an unenhanced chest low-dose computed tomography (LDCT). The need for oxygen therapy, transfer to the intensive care unit (ICU), death, and overall length of stay in hospital (for in-patients) were documented. Virological follow-up included ≥1 test(s) done systematically on days 2, 6 and 10. Patients with persistent positive PCR on day 10 were proposed further testing every 4 days until the test became negative.
2.3. COVID-19 treatment and outcomes
Patients with no contraindications [13,14] were proposed a combination of 200 mg of oral HCQ, three times daily for ten days combined with five days of AZ (500 mg on day 1 followed by 250 mg daily for the next four days). Therapy was not supervised. No children <14 years, pregnant women or patients with G6PD deficiency (based on patient’s declaration only) were included. The systematic pre-therapy workup included serum electrolyte analysis, and an electrocardiogram with corrected QT measurement (Bazett’s formula). A specific inclusion protocol and follow-up for torsade de pointes risk was designed. Any drug, being used by the patient, with the potential to prolong the QT interval and non-vital potassium-depleting drugs (diuretics prescribed for high blood pressure) were systematically stopped. When potassium-depleting drugs could not be stopped or in case of documented hypokalaemia at admission, potassium supplementation was provided and HCQ was administered only when the potassium level was normalized. Close serum electrolyte analysis monitoring was performed in patients with low serum potassium levels at baseline. An electrocardiogram was routinely performed 48 h after the start of treatment. Treatment with HCQ was discontinued when the corrected QT interval (QTc, Bazett’s formula) was > 500ms and the risk-benefit ratio of HCQ+AZ treatment was estimated by the infectious disease specialist and agreed with the cardiologist, at between 460 and 500ms. The indications for this control ECG were restricted after an initial workup in 848 ECG from 424 patients (at day 0 and day 2 for each patient) showing that all contraindicative repolarization abnormalities had been detected on the first ECG.
HCQ dosage was performed as previously described [14,21] and a concentration of > 0.1 μg/mL was considered in the therapeutic range [22]. Broad spectrum antibiotics (ceftriaxone or ertapenem) were added for patients with pneumonia and NEWS score ≥ 5. Symptomatic treatments, including notably oxygen, were added as needed. The primary outcomes were i) an aggressive clinical course requiring oxygen therapy, transfer to the ICU or death after at least three days of treatment, and prolonged hospitalization (10 days or more), and ii) contagiousness as assessed by PCR and culture.
2.4. Additional investigations on patients with treatment failure
Patients with clinical or virological failures were accurately characterized and a close clinical and viral follow-up was performed overtime. We defined a group with poor clinical outcome (PClinO) by either death or transfer to ICU or hospitalization for 10 days or more and a group with poor virological outcome (PVirO) was defined by viral shedding persistence at day 10. Finally, individuals who belonged neither to the PClinO group nor the PVirO group were attributed to a group with a good outcome (GO). Factors associated with clinical failure were identified by comparing the PClinO to the GO group and factors associated with virological failure were identified by comparing the PVirO group to the GO group. We performed additional tests on patients with atypical evolution including late SARS-CoV-2 cultures on Vero E6 cells, as previously described [23], and broad-spectrum detection of other viruses by multiplex PCR [19] in respiratory samples. In addition, cDNA was reverse transcribed directly from total viral SARS-CoV-2 RNA rhinopharyngeal samples following the manufacturer’s recommendations. cDNAs were purified by using Agencourt AMPure beads (Beckman Coulter, Villepinte, France). Genomic DNA was extracted using the EZ1 biorobot with the EZ1 DNA tissue kit (Qiagen, Hilden, Germany) and then sequenced on a MiSeq sequencer (Illumina Inc, San Diego, CA,USA) with the Nextera Mate-Pair sample prep and Nextera XT Paired End kits (Illumina Inc., San Diego, CA, USA). The SARS-CoV-2 genomes were downloaded from NCBI (https://www.ncbi.nlm.nih.gov/) or are available at EMBL-EBI under the BioProject: PRJEB37693. Phylogenetic reconstruction was performed using NEXSTRAIN (https://nextstrain.org/) and GISAID (Global Initiative; https://www.gisaid.org/) [24].
2.5. Statistical methods
Continuous and categorical variables were presented as mean (std), median, min-max and n (%), respectively. We used the Student t-test, Mann-Whitney U test, Chi-square test, or Fisher’s exact test to compare differences between the three groups (GO, PVirO, and PClinO) where appropriate. The GO group was chosen as the reference group for statistical testing (PVirO vs. GO and PClinO vs. GO respectively). To explore risk factors associated with the PVirO and PClinO groups, we also performed multivariable analyses using logistic regression models. All variables significant at p < .01 in univariate analyses were introduced in the initial multivariate model. A stepwise approach was then used to assess the iteration of variables and to control potential confounders (both values of significance level for entry and stay were set at 0.05.) A two-sided alpha of less than 0.05 was considered statistically significant. All analyses were carried out using SAS 9.4 statistical software (SAS Institute, Cary, NC).
2.6. Ethics statement
Data presented herein were collected retrospectively from routine care using the electronic health recording system of the hospital according to the MR-004 reference methodology for the processing of personal data. Accessibility to data is protected according to European General Data Protection Regulation No 2016/679. The non-interventional retrospective nature of the study has been approved by our institutional review board committee (Mediterranée Infection N°: 2020–13). At the time the study was conducted, HCQ was approved for COVID-19 as a hospital delivery only, in France. For all patients, the prescription of HCQ+AZ was made during either complete hospitalization or at day-care hospital by one of the practicing physicians, independently of the investigator, after collegial decision based on the most recent scientific data available and after assessment of the benefit/harm ratio of the treatment in accordance with the provisions of the Code of Ethics (Article R. 4127-8 of the Public Health Code). No supplementary monitoring or diagnostic procedures were added to normal clinical practice allowing surveillance and management of patient (monitoring of HCQ levels and SARS-CoV-2 viral load surveillance and ECG).
3. Results
3.1. Participants
Among 1,411 eligible patients with available data, 350 were excluded (Fig. 1, Table 1). For the present analysis, a total of 1,061 patients were treated at least 3 days with the combination of HCQ+AZ at IHU, including 492 male (46.4%). The mean age was 43.6 years (standard deviation (sd), 15.6 years). Underlying conditions and symptoms declared by the patients (91.7%) are described in Table 2. The majority (95.0%) of patients had a low NEWS score. The time between the onset of the symptoms and the first day of treatment (day 0) was 6.4 days (standard deviation, 3.8 days). A total of 469 patients (65.7%) had a LD CT scan consistent with pneumonia including 20.5% and 2.2% with a medium and severe score, respectively. The mean viral load obtained by PCR on nasopharyngeal swab at day 0 was 26.6 Ct with 5.0 as standard deviation.
Table 1. Reasons for exclusion of 350 patients from the study.
| 94 previously published | [13,14] |
|---|---|
| 33 with cardiac contraindication | 11 non specified 10 prolonged QTc 3 Brugada syndrome 1 myocarditis history 1 left ventricular hypertrophy 1 severe ischemic cardiopathy 1 left bundle branch block 1 right bundle branch block 1 atrio-ventricular block 1 supraventricular tachycardia 1 ECG abnormalities suggesting underlying cardiac ischemic disease 1 unspecified arrhythmia |
| 28 considered cured by the physician based on clinical feature | |
| 21 refusal of hydroxychloroquine or azithromycin treatment | |
| 15 with potential risk for drug interactions with hydroxychloroquine or azithromycin treatment | Cardiac drugs 3 flecainide 2 amiodarone 1 bisoprolol 1 nicardipine Neuropsychiatric drugs 2 escitalopram 1 levetiracetam 1 cyamemazine 1 venlafaxine 1 lamotrigine 1 valproate 1 lithium Others 1 cabergoline 1 dolutegravir/rilpivirine |
| 10 hypokaliemia | |
| 6 children < 15 years | |
| 6 ophtalmologic contraindication to hydroxychloroquine treatment | 3 retinopathy 2 glaucoma 1 accomodation disorder |
| 4 known allergy to hydroxychloroquine or azithromycin treatment | |
| 2 breastfeeding | |
| 2 gastrointestinal intolerance to hydroxychloroquine or azithromycin treatment | |
| 2 swallowing disorders | |
| 1 insomnia | |
| 61 under hydroxychloroquine only before the publication of the first study [13] that led to the systematic use of dual therapy with azithromycin on March 20, 2020. | |
| 66 unspecified |
The reasons mentioned here are those retained by physicians who have seen the patients and do not necessarily correspond to formal contraindications. Several reasons may coexist in a same patient.
Table 2. Baseline characteristics according to clinical and virological outcome of 1061 patients treated with HCQ+AZ ≥ 3 days at IHU Méditerranée infection Marseille, France with day 0 between March 3 and March 31, 2020.
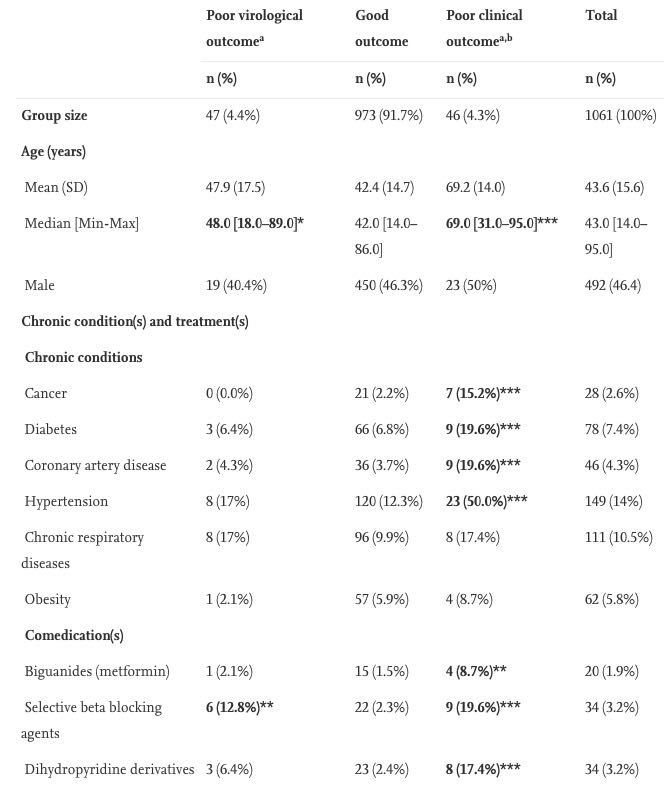


Poor virological outcome (PVirO): viral shedding persistence at day 10; Poor clinical outcome (PClinO): either death or transfer to intensive care unit (ICU) or hospitalization for 10 days or more; Good outcome: individuals who belonged neither to the PClinO group nor the PVirO group. SD: standard deviation. aFive patients belonged to both the PVirO and PClinO outcome so the sum of frequencies may be above 1061. bIncluding 8 deaths. cData available for 928 patients (56 patients who did not declare any symptom before treatment start were excluded and 77 with missing data), dfor 714 patients, efor 992 patients and ffor 263 patients. On low-dose pulmonary CT-scanner, patients were classified as no involvement (lack of lung involvement (ground glass opacities, consolidation or crazy paving pattern); minimal involvement (subtle ground glass opacities); intermediate involvement (less than 50% of segment involvement in no more than 5 segments) and severe involvement (involvement of more than 5 segments). The denominator was mentioned when the result was not available for all patients. *p < 0.05; **p < 0.01; ***p < 0.001 (Fisher’s exact test, Student t-test, Wilcoxon-Mann-Whitney where appropriate; reference group is good outcome).
Successful isolation of virus in cell culture was obtained from 204 patients among 915 tested (22.3%) on nasopharyngeal sample collected before treatment. A total of 973 patients (91.7%) had a good clinical outcome (GO). Among 263 patients tested at day 2, HCQ was low (<0.1 μg/mL) in 30 patients including 3 in which it was undetectable. The vast majority of patients did not report any adverse event that could be attributed to their treatment (97.6%). Twenty five patients reported mild adverse events, and three discontinued their treatment (Table 3).
Table 3. Adverse events.
| Patients without any adverse event | 1036 (97.6%) |
| Patients with adverse events possibly related to the treatmenta | 25 (2.4%) |
| Diarrhea | 12 |
| Abdominal pain | 3 |
| Headache | 3 |
| Nausea | 2 |
| Insomnia | 2 |
| Transient blurred vision | 2 |
| Vomiting | 1 |
| Urticaria | 1 |
| Erythematous and bullous rash | 1 |
| Discontinuation of treatment | 3 (abdominal pain, urticaria, erythematous and bullous rash) |
a
Some patients reported more than one adverse event.
Nine patients had a QTc prolongation of more than 60 ms from baseline but no patient exceeded 500 ms, which corresponds to the threshold contraindicating treatment. No rhythmic cardiac events or sudden deaths were observed.
3.2. Poor clinical outcome
Forty-six patients (4.3%) were classified into the PClinO group including 10 patients transferred into ICU of whom 2 died, 6 who died in conventional hospital units, and 30 additional patients who were hospitalized for 10 days or more (update April 18th). Their median age (69.0 years; 31–95 years) was significantly higher than that of patients included into the GO group (42.0 years; 14–86, p < .001) (Table 2). Sex ratio (M/F) was 1. When compared with patients in the GO group, PClinO group patients were significantly more likely to report previous hypertension (50%), diabetes (19.6%), coronary artery diseases (19.6%) and cancer (15.2%) (p < .001). In addition, they were more likely to receive beta-blocking agents, dihydropyridine derivatives, angiotensin II receptor blockers, and HMG-CoA reductase inhibitors (p < .001), diuretics (p < .001) and metformin (p < .01). The time between onset of symptoms and the beginning of the treatment was shorter and their NEWS score was less likely to be low than in the GO group patients (Table 2). They were less likely to present with normal CT-scan at admission (p < .001). Interestingly, the mean HCQ dosage at day 2 (0.20 μg/ml (0.17)) was significantly lower than in the GO group (p < .01, Table 2) with 12/37 tested cases with a dosage lower than 0.100 μg/mL (p < .001), and 3 without detectable HCQ. However, upon multivariate analysis, only older age (OR = 1.11: 1.07–1.15), selective beta blocking agents (OR = 4.16: 1.19–14.55), angiotensin II receptor blockers (OR = 18.40: 6.28–53.90) and medium and high NEWS scores (OR = 9.48: 3.25–27.66; OR = 10.05: 3.16–32.02, respectively) were significantly associated with the poor clinical outcome (Table 4). When adjusting for hypertension in multivariate analysis, the two variables angiotensin II receptor blockers and selective beta blockers remained statistically associated with PClinO and PVirO. With a model selecting only people with hypertension, these two molecules remained significantly associated to the PClinO but not the PVirO outcome (angiotensin II receptor blockers, point estimate 34.7, 95% CI 4.98–241.6 – selective beta blockers, 26.6, 95%CI 4.81–146.9). Low dose CT scan score revealed pneumonia in 35 PClinO group patients (90%). Three severe patients were treated by anti-IL1 (anakinra) and none of them died. No patients were treated with steroids. High dose preventive or curative anticoagulants were administered for severe patients.
Table 4. Multivariable logistic regressions of variables found statistically different in the univariate analysis.

NS: not statistically significant (p > 0.05) after stepwise selection.a
Missing values (n = 69) were imputed based on the mean value (mean = 26.6, see Table 1).
Regarding specifically the 8 patients who died after having received HCQ+AZ ≥ 3 days, their median age was 79 years (74–95 years) (Table 5). Six patients (75%) reported hypertension and one active cancer. Severity at admission was observed with a NEWS score ranging from 5 to 11 (mean 7.75) and low dose CT scan performed on 4 patients revealed intermediate to severe pneumonia involvement. All deaths resulted from respiratory failure and not from sudden death. All had repeated ECG with none showing torsades de pointe. Finally, mean HCQ dosage at day 2 was 0.162 including one patient with a blood level lower than 0.10 μg/mL. As of 18th of April, 2020, 33 of 46 patients in the PClinO group are now cured. Accordingly, 1048 (98.7%) of patients who received the HCQ+AZ combination are cured so far.
Table 5. Clinical data of eight patients who died from COVID19 infection out of 1,061 treated with hydroxychloroquine or azithromycin for at least three days. Day 0 between March 3rd and March 31, 2020; Follow up regarding fatal issue: April 18th, 2020.
| Age, median (min-max) | 79 (74–95) |
| Chronic condition | |
| Hypertension, N (%) | 6 (75%) |
| Cancer, N (%) | 1 (12.5%) |
| NEWS score, mean (min-max) | 7.75 (5–11) |
| Time between symptoms and hospitalization, mean (min-max) | 5.6 days (2-14) |
| Time between hospitalization and death, mean (min-max) | 16 days (6-26) |
| Day 2-hydroxychloroquine blood level (μg/mL), mean (min-max) | 0.162 (0.071–0.338) |
3.3. Viral clearance
Forty-seven patients, including 5 who were also PClinO, exhibited a persistent nasal viral carriage at completion of treatment. Their sex ratio (M/F) and mean age were 0.68 and 47.9 ± 17.5 years old, respectively. Of the 21 PVirO patients for whom specimens were available after day 10, 20 had negative viral loads by day 15 post onset of treatment (95.2%). In addition, all eleven patients for whom daily culture was attempted were negative by day 10. When compared to GO group patients in this study, PVirO group patients were older, more likely to use selective beta blocking agents and angiotensin II receptor blockers. They also exhibited a significantly higher viral load (p < .01) at diagnosis, were less likely to have a low NEWS score, and they were treated earlier (Table 2). However, in multivariate analysis, time between onset of symptoms and first day of treatment start did not remain significantly associated with viral shedding persistence. The proportion of persistent viral shedders was higher in patients with poor clinical outcome (5/46 (10.8%)) than in patients without good clinical outcome (42/1015 (4.1%)), one-sided mid-p exact test, p = .03).
In order to determine whether virus carriage persistence was associated with another concurrent infection, we tested 8 PVirO individuals using the FTD 21 Plus kit (Fast Track Diagnostics, Luxembourg). Two of these eight patients, sampled on March 21st and 24th 2020, respectively, were positive for bocavirus. All other tested pathogens were negative. Then, in order to determine whether other patients sampled during the same timeframe might have been also infected, we selected among good outcome patients 112 individuals who had been sampled between March 21st and 24th, 2020. None of them were positive for bocavirus or any other viruses (p < .001, Fisher exact test). Whether this co-infection played a role in viral persistence is as-yet unknown. Comparative genomics between viral isolates from 3 non-treatment-responding patients (both PVirO and PClinO), one PClinO patient, one PVirO patient and 10 treatment-responding patients as well as 56 SARS-CoV-2 strains from various geographical origins did not identify any specific viral variant linked to resistance to treatment (Fig. 2).


4. Discussion
The efficacy of the combination of HCQ and AZ against COVID-19 has become a very controversial issue in the medical community, leading to many leaked social media reports and speeches from politicians. Evidence is needed to augment the knowledge of outcomes of patients with COVID-19 who are treated with this drug combination. In our analysis, which is not a RCT but which relates the real-life experience of physicians treating patients in the context of an emerging pandemic, we report the outcomes of 1061 COVID-19 patients treated with an HCQ+AZ combination from the time of diagnosis. The spectrum of severity of COVID-19 ranges from mild symptoms to severe respiratory distress [1]. We assessed patients who received at least three days of treatment and eight days of follow-up. The majority of patients in our work had relatively mild disease at admission (95%). Under these conditions, the treatment was associated with a low proportion of patients with worsening of the disease, as only 10 patients (0.9%) were transferred to the intensive care unit and a low proportion of death, as only eight (0.75%) patients died (case fatality rate updated April 18th, 2020). It was also associated with a low frequency of persistent viral shedding. In our experience, the treatment was well tolerated with only a low proportion of adverse events (2.4%), all of which were mild with three discontinuations of treatment (0.3%) [25].
Regarding viral shedding persistence, we observed that it was 4.4% at day 10 in treated patients, which is extremely low in comparison to Chinese studies, the largest of which showed that viruses are shed on average for 20 days with extremes of up to 38 days [1]. This may have important consequences in terms of contagiousness of the disease. We did not find any specificity in the genomes of viruses in patients with viral shedding persistence.
We were surprised to find in the PClinO group that HCQ blood levels were lower than therapeutic target in 32.4% cases including two patients without any drug in the blood. We cannot exclude that some of these patients were not adherent with the prescribed treatment since therapy intake was not controlled. We therefore recommend that close control of HCQ blood level be performed in treated patients so that drug dosage could be adapted accordingly.
As already described by others [1,26], we confirm that COVID-19 patients with PClinO are significantly more likely to be elderly patients. Moreover, when COVID-19 patients were treated belatedly and already showing clinical or radiological signs of pneumonia, the prognosis was poorer but genomes of viruses associated with PClinO were not apparently different from those in other patients (Fig. 2). Multivariate analysis showed that selective beta-blocking agents and angiotensin II receptor blockers were independent factors associated with poor clinical and virological outcomes (p < .05).
Our study has some limitations. Because services were overwhelmed, data was incomplete on some patients. CT-scans and serum drug levels were not available for all patients, notably in those admitted out of hours.
As a conclusion, based on our experience, we consider reasonable to follow the recommendations made in Asian countries for the control of COVID-19, notably in Korea and China that consist in early testing as many patients as possible and treating them with available drugs where this strategy has produced much better results than in countries where no active policy has been implemented outside containment. In China, drugs that were recommended were primarily HCQ but also α-interferon, lopinavir, ritonavir and umifenovir [27], in Korea, recommended drugs were lopinavir/ritonavir and chloroquine [28]. In the context of a pandemic with a lethal respiratory virus, we believe that early detection of positive cases and carefully controlled treatment with safe and well-tolerated drugs should be generalized in outpatient medicine, i.e. in individuals with mild symptoms before signs of severity appear. Strict attention should be paid to contraindications and possible interactions with concomitant medication. Finally, there is a need to repurpose existing drugs and evaluate these in controlled trials where possible in the constraints of a pandemic.
Author’s Note: Since this analysis was completed, and as of the 29th of April, 2020, two more patients in the PClinO group died resulting in an overall 0.9% case fatality rate (CFR) for these 1061 patients.
Funding
This work was funded by ANR-15-CE36-0004-01 and by ANR “Investissements d’avenir”, Méditerranée infection 10-IAHU-03, and was also supported by Région Provence-Alpes-Côte d’Azur. This work had received financial support from the Mediterranean Infection Foundation.
CRediT authorship contribution statement
Matthieu Million: Conceptualization, Formal analysis, Writing – original draft. Jean-Christophe Lagier: Conceptualization, Formal analysis, Writing – original draft. Philippe Gautret: Formal analysis, Writing – original draft. Philippe Colson: Conceptualization, Formal analysis, Writing – original draft. Pierre-Edouard Fournier: Conceptualization, Formal analysis, Writing – original draft. Morgane Mailhe: Conceptualization, Formal analysis, Writing – original draft. Vera Esteves-Vieira: Conceptualization. Florian Correard: Conceptualization. Audrey Giraud-Gatineau: Conceptualization. Yanis Roussel: Conceptualization. Stéphane Honoré: Conceptualization, Formal analysis. Alexis Jacquier: Conceptualization. Jean-Claude Deharo: Conceptualization. Eric Chabrière: Conceptualization. Anthony Levasseur: Conceptualization. Florence Fenollar: Conceptualization. Jean-Marc Rolain: Conceptualization, Formal analysis. Yolande Obadia: Conceptualization, Formal analysis. Philippe Brouqui: Conceptualization, Formal analysis. Michel Drancourt: Conceptualization, Formal analysis. Bernard La Scola: Conceptualization, Formal analysis. Philippe Parola: Conceptualization, Formal analysis, Writing – original draft. Didier Raoult: Conceptualization, Formal analysis, Writing – original draft.
Declaration of competing interest
The authors declare no competing interests. Funding sources had no role in the design and conduct of the study; collection, management, analysis, and interpretation of the data; and preparation, review, or approval of the manuscript. Our group used widely available generic drugs distributed by many pharmaceutical companies (Supplementary data).
Acknowledgments
We are thankful to Marion Bechet, Pascal Chanez, Véronique Filosa, Marc Gainier, Marion Gouitaa, Marie-Thérèse Jimeno, Cléa Melenotte, Matthieu Bardou, Marc Léone, Jean-Robert Harlé, Veronique Veit, all medical students from Aix Marseille University, all nurses, laboratory staff, administrative, technical and security staff of Assistance Publique-Hôpitaux de Marseille and IHU Méditerranée Infection, all medical doctors volunteers, and the Bataillon des Marins Pompiers de Marseille for their help. We thank the 6 reviewers who helped to substantially improving and clarifying the manuscript with their many comments and suggestions.
Appendix A. Supplementary data
The following is the Supplementary data to this article:Download : Download Word document (29KB)
Multimedia component 1.
References
[1]F. Zhou, T. Yu, R. Du, G. Fan, Y. Liu, Z. Liu, et al.Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort studyLancet, 395 (2020), pp. 1054-1062Article Download PDF View Record in ScopusGoogle Scholar
[2]X. Yao, F. Ye, M. Zhang, C. Cui, B. Huang, P. Niu, et al.In vitro antiviral activity and projection of optimized dosing design of hydroxychloroquine for the treatment of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)Clin Infect Dis (2020), p. 5801998pii:ciaa237 Google Scholar
[3]J. Liu, R. Cao, M. Xu, X. Wang, H. Zhang, H. Hu, et al.Hydroxychloroquine, a less toxic derivative of chloroquine, is effective in inhibiting SARS-CoV-2 infection in vitroCell Discov, 6 (2020), p. 16Cross Ref View Record in Scopus Google Scholar
[4]S. Weston, C.M. Coleman, R. Haupt, J. Logue, K. Matthews, M. FriemanBroad anti-coronaviral activity of FDA approved drugs against 1 SARS-CoV-2 in vitro and SARS-CoV in vivobioRxiv (2020), 10.1101/2020.03.25.008482 Google Scholar
[5]F. Touret, R. Gilles, K. Barral, A. Nougairede, E. Decroly, X. De Lamballerie, et al.In vitro screening of a FDA approved chemical library reveals potential inhibitors of SARS-CoV-2 replicationbioRxiv (2020), 10.1101/2020.04.03.023846 Google Scholar
[6]J. Andreani, B.M. Le, I. Duflot, P. Jardot, C. Rolland, M. Boxberger, et al.In vitro testing of combined hydroxychloroquine and azithromycin on SARS-CoV-2 shows synergistic effectMicrob Pathog (2020), p. 104228Article Download PDF Google Scholar
[7]Z. Chen, J. Hu, Z. Zhang, S. Jiang, S. Han, D. Yan, et al.Efficacy of hydroxychloroquine in patients with COVID-19: results of a randomized clinical trialmedRxiv (2020), 10.1101/2020.03.22.20040758Google Scholar
[8]W. Tang, Z. Cao, M. Han, Z. Wang, J. Chen, W. Sun, et al.Hydroxychloroquine in patients with COVID-19: an open-label, randomized, controlled trialmedRxiv (2020), 10.1101/2020.04.10.20060558 Google Scholar
[9]M.A. Ashraf, N. Shokouhi, E. Shirali, F. Davari-Tanha, O. Memar, A. Kamalipour, et al.COVID-19 in Iran, a comprehensive investigation from exposure to treatment outcomesmedRxiv (2020), 10.1101/2020.04.20.20072421 Google Scholar
[10]J. Chen, D. Liu, L. Liu, P. Liu, Q. Xu, L. Xia, et al.A pilot study of hydroxychloroquine in treatment of patients with common coronavirus disease-19 (COVID-19)J Zhejiang Unniv (Med Sci), 49 (2020)0 Google Scholar
[11]M. Mahevas, V.T. Tran, M. Roumier, A. Chabrol, R. Paule, C. Guillaud, et al.No evidence of clinical efficacy of hydroxychloroquine in patients hospitalised for COVID-19 infection and requiring oxygen: results of a study using routinely collected data to emulate a target trialmedRxiv (2020), 10.1101/2020.04.10.20060699 Google Scholar
[12]J. Magagnoli, S. Narendran, F. Pereira, F. Cummings, J.W. Hardin, S. Scott Sutton, et al.Outcomes of hydroxychloroquine usage in United States veterans hospitalized with Covid-19medRxiv (2020), 10.1101/2020.04.16.20065920Google Scholar
[13]P. Gautret, J.C. Lagier, P. Parola, V.T. Hoang, L. Meddeb, M. Mailhe, et al.Hydroxychloroquine and azithromycin as a treatment of COVID-19: results of an open-label non-randomized clinical trialInt J Antimicrob Agents (2020), p. 105949, 10.1016/j.ijantimicag.2020.105949[Epub ahead of print] Article Download PDF Google Scholar
[14]P. Gautret, J.C. Lagier, P. Parola, V.T. Hoang, L. Meddeb, J. Sevestre, et al.Clinical and microbiological effect of a combination of hydroxychloroquine and azithromycin in 80 COVID-19 patients with at least a six-day follow up: an observational studyTrav Med Infect Dis (2020 Apr 11), p. 101663, 10.1016/j.tmaid.2020.101663[Epub ahead of print]ArticleDownload PDFGoogle Scholar
[15]H. Retallack, L.E. Di, C. Arias, K.A. Knopp, M.T. Laurie, C. Sandoval-Espinosa, et al.Zika virus cell tropism in the developing human brain and inhibition by azithromycinProc Natl Acad Sci U S A, 113 (2016), pp. 14408-14413CrossRefView Record in ScopusGoogle Scholar
[16]P.B. Madrid, R.G. Panchal, T.K. Warren, A.C. Shurtleff, A.N. Endsley, C.E. Green, et al.Evaluation of Ebola virus inhibitors for drug repurposingACS Infect Dis, 1 (2015), pp. 317-326 Cross RefV iew Record in Scopus Google Scholar
[17]E. Bosseboeuf, M. Aubry, T. Nhan, J.J. dde Pin, J.M. Rolain, D. Raoult, et al.Azithromycin inhibits the replication of Zika virusJ Antivir Antiretrovir, 10 (2018), pp. 6-11View Record in ScopusGoogle Scholar[18]Sermo SermoCOVID-19 real time barometer(2020)https://app.sermo.com/covid19-barometer?utm_campaign=wwwsermo_covid19, Accessed 17th Apr 2020Last accessed:Google Scholar[19]S. Amrane, H. Tissot-Dupont, B. Doudier, C. Eldin, M. Hocquart, M. Mailhe, et al.Rapid viral diagnosis and ambulatory management of suspected COVID-19 cases presenting at the infectious diseases referral hospital in Marseille, France, – January 31st to March 1st, 2020: a respiratory virus snapshotTrav Med Infect Dis (2020 Mar 20), p. 101632, 10.1016/j.tmaid.2020.101632[Epub ahead of print]Article Download PDF Google Scholar
[20]X. Liao, B. Wang, Y. KangNovel coronavirus infection during the 2019-2020 epidemic: preparing intensive care units-the experience in Sichuan Province, ChinaIntensive Care Med, 46 (2020), pp. 357-360CrossRefView Record in ScopusGoogle Scholar
[21]N. Armstrong, M. Richez, D. Raoult, E. ChabriereSimultaneous UHPLC-UV analysis of hydroxychloroquine, minocycline and doxycycline from serum samples for the therapeutic drug monitoring of Q fever and Whipple’s diseaseJ Chromatogr B Analyt Technol Biomed Life Sci, 1060 (2017), pp. 166-172ArticleDownload PDFView Record in ScopusGoogle Scholar
[22]J.C. Lagier, F. Fenollar, H. Lepidi, R. Giorgi, M. Million, D. RaoultTreatment of classic Whipple’s disease: from in vitro results to clinical outcomeJ Antimicrob Chemother, 69 (2014), pp. 219-227CrossRefView Record in Scopus Google Scholar
[23]B. La Scola, M. Le Bideau, J. Andreani, V.T. Hoang, C. Grimaldier, P. Colson, et al.Viral RNA load as determined by cell culture as a management tool for discharge of SARS-CoV-2 patients from infectious disease wardsEur J Clin Microbiol Infect Dis (2020), 10.1007/s10096-020-03913-9 Google Scholar
[24]J. Hadfield, C. Megill, S.M. Bell, J. Huddleston, B. Potter, C. Callender, et al.Nextstrain: real-time tracking of pathogen evolutionBioinformatics, 34 (2018), pp. 4121-4123Cross Ref View Record in Scopus Google Scholar
[25]J.C.E. Lane, J. Weaver, K. Kostka, T. Duarte-Salles, M.T. Abrahao, H. Alghoul, et al.Safety of hydroxychloroquine, alone and in combination with azithromycin, in light of rapid wide-spread use for COVID-19: a multinational, network cohort and self-controlled case series studymedRxiv (2020), 10.1101/2020.04.08.20054551 Google Scholar
[26]Z. Wu, J.M. McGooganCharacteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72314 cases from the Chinese center for disease control and preventionJ Am Med Assoc (2020 Feb 24), 10.1001/jama.2020.2648[Epub ahead of print] Google Scholar
[27]L. Dong, S. Hu, J. GaoDiscovering drugs to treat coronavirus disease 2019 (COVID-19)Drug Discov Ther, 14 (2020), pp. 58-60Cross Ref View Record in Scopus Google Scholar
[28]K. Sung-sunPhysicians work out treatment guidelines for coronavirusKorea Biomedical Review (2020)http://m.koreabiomed.com/news/articleView.html?idxno=7428 Google Scholar
See the original source here: https://www.sciencedirect.com/science/article/pii/S1477893920302179

